Customized Training for the Career You Want
Because our fellows come from a variety of specialties, we focus on individualized learning and career planning.
This includes frequent and formative feedback, ongoing faculty and peer mentorship, and dedicated curricular time.
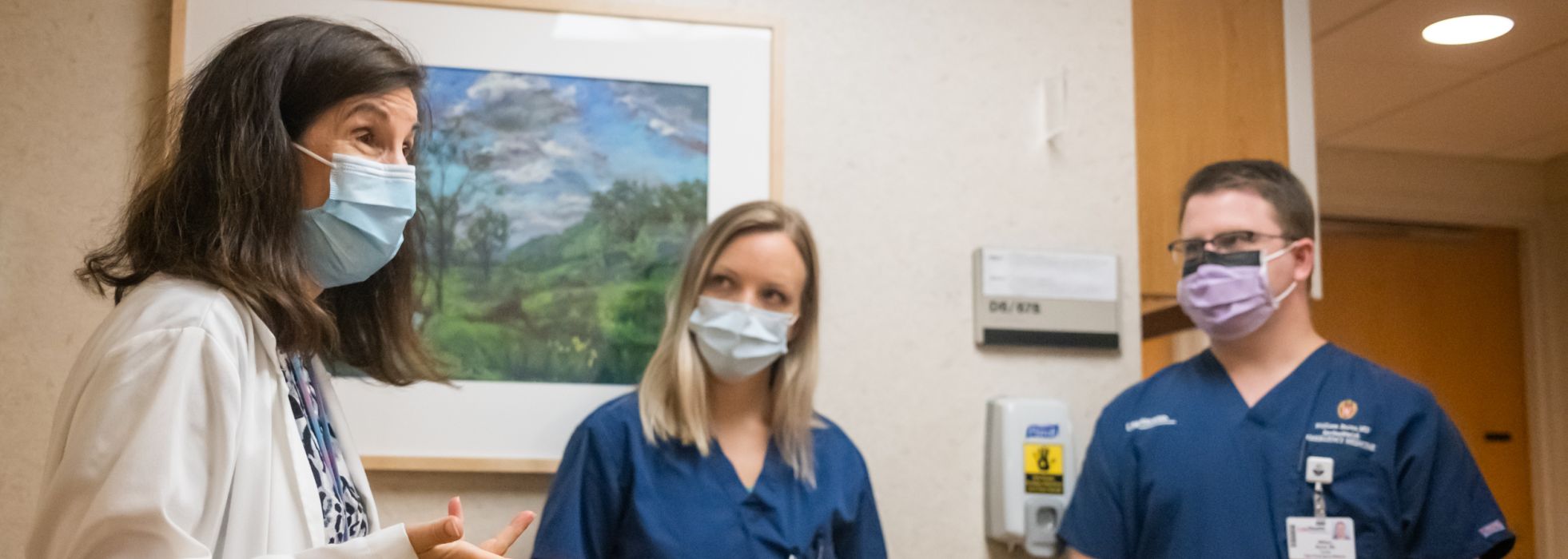
Our dedicated interprofessional educators span four training sites: UW Health, American Family Childrens' Hospital, the William S. Middleton Memorial VA Hospital, and Agrace Hospice.
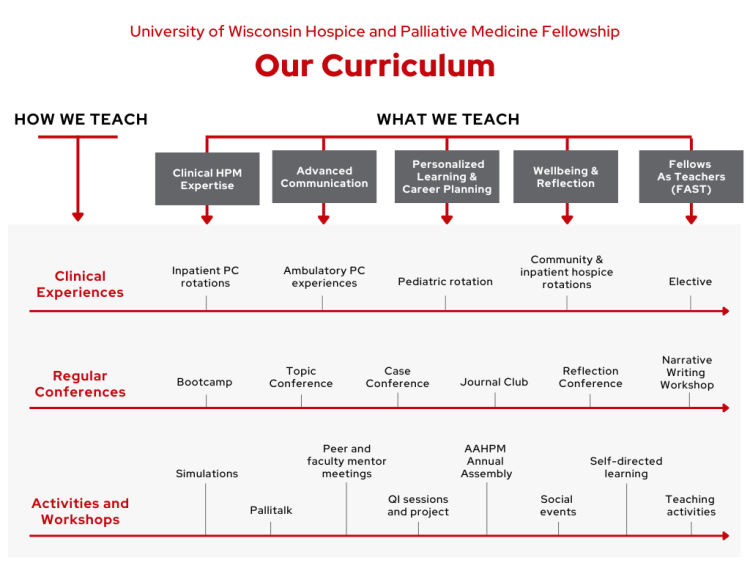
Didactic Experiences
- Advanced communication training, including the UW-developed "Best Case/ Worst Case" tool (see video)
- Well-being and resiliency curriculum that includes narrative writing workshops
- High-yield conferences: topic conferences, case conferences, and Journal Club
- A supportive learning environment that emphasizes learning by doing: family meeting simulations, acute case simulations and PalliTALK, our regional fellow communication workshop
Clinical Experiences
Scholarly Activity
Research
All of our fellows participate in a faculty-supported QI curriculum and project, and present at the UW Health QI Symposium.
If you are interested in research, there are opportunities to partner with faculty. You can also continue your scholarly work through an optional second-year VA advanced fellowship.
Teaching
Our learners are also teachers. We developed a unique Fellows as Teachers curriculum to grow our field and train the next generation of HPM educators. See our Teaching page for details.
We also offer an option for a second year focused on medical education and leadership.
Additional Opportunities in the Department
- QI Curriculum for Fellowship. Teaches fellows how to apply quality improvement knowledge and skills directly to clinical practice.
- Wisdom, Integrity, Leadership and Development (WILD). Program that provides fellows from all backgrounds with skills to advance their careers and become leaders in academic medicine.