Discover What Sets Us Apart
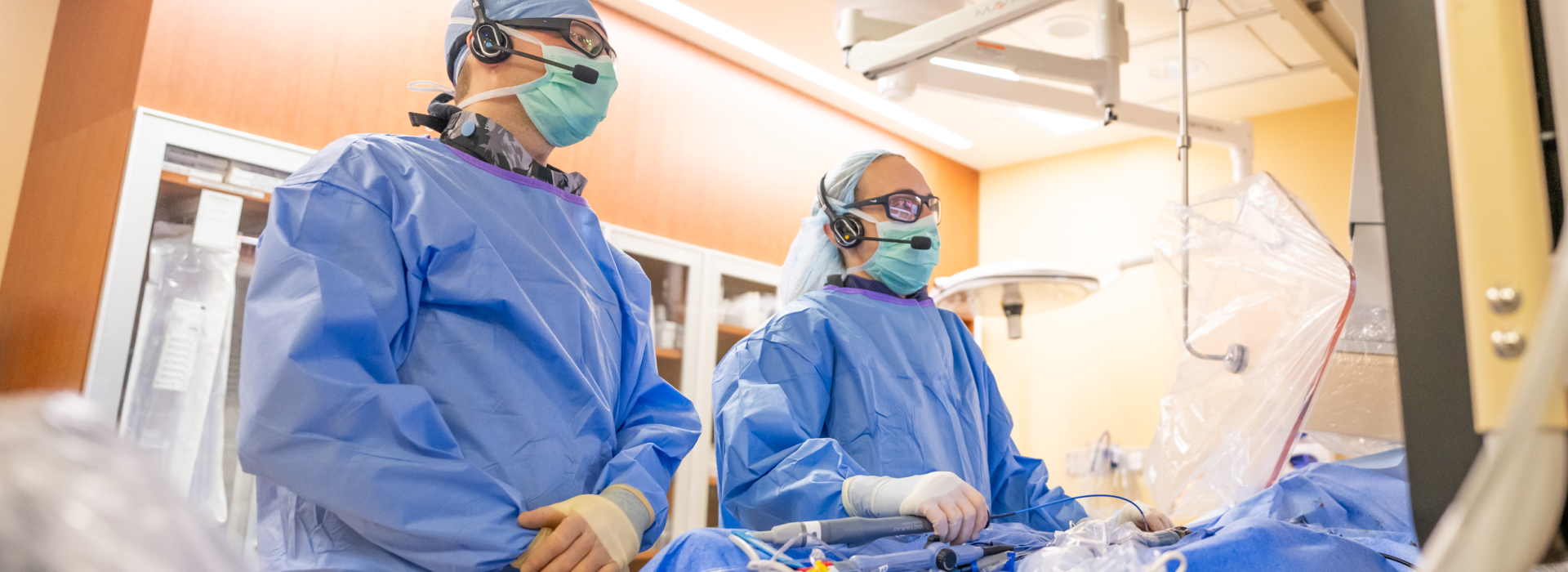
Choose Your Path
Build your ideal education with our comprehensive clinical training, individualized approach to curriculum and focused tracks and pathways.
I’ve made some of my closest friends in this program and have had mentors who have gone above and beyond to support me—people I’ve looked up to for years who have taken the time to invest in my career and development.


Thrive in our Supportive Environment
Here, we create welcoming, affirming experiences for all. Join us and flourish.
Meet Our Program Director
"Our comprehensive clinical experiences will make you an outstanding internist, no matter where your career takes you. Our learners and faculty partner to help you become the best physician you can be.
I’m an educator at heart. I love having longitudinal relationships with residents, teaching and modeling skills, seeing professional identities form, and celebrating successes. I look forward to getting to know you!"



Life in Madison
Madison is a place unlike anywhere else. Find out why we love living here.
Education News
Questions?
Please contact us with any questions about our program.










